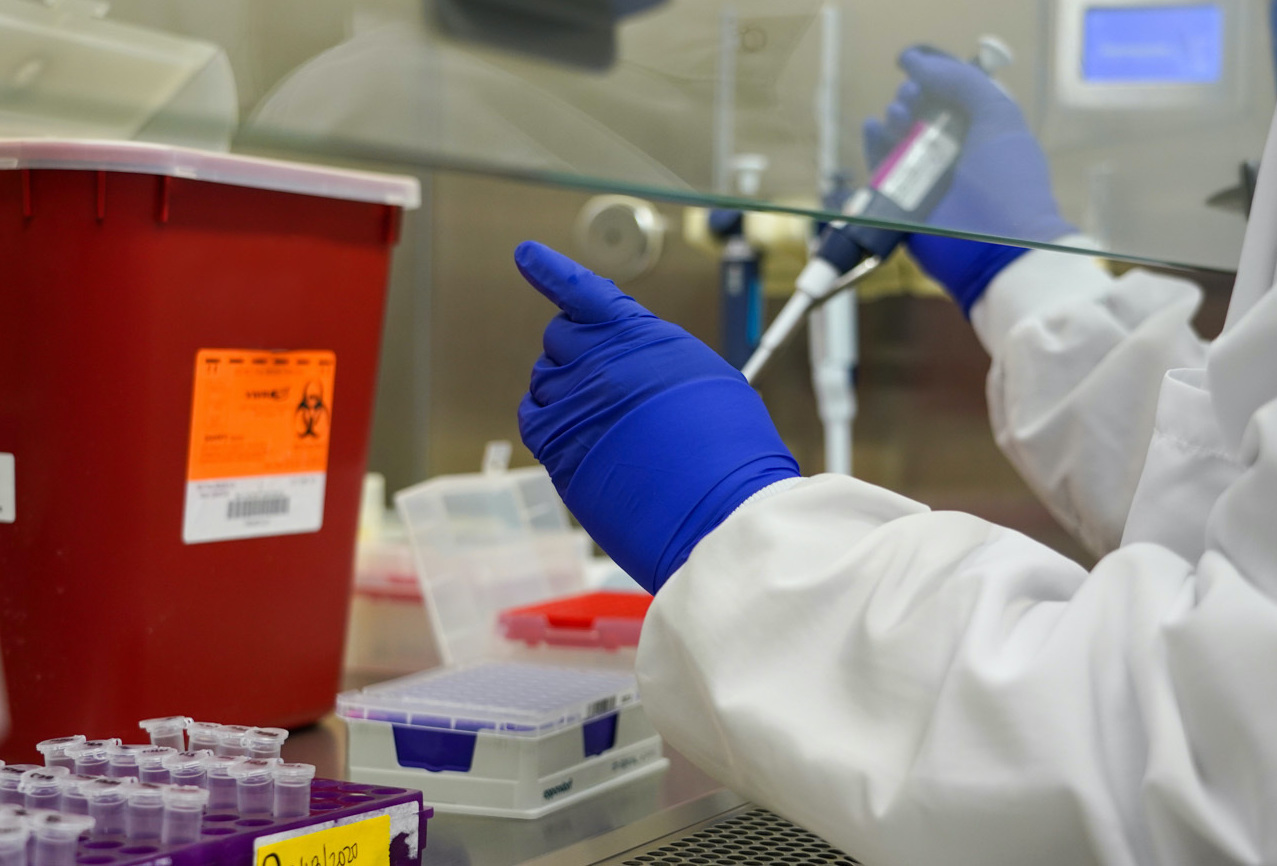
SAN DIEGO — Before leaving Southern California last week for predeployment training, the crew of aircraft carrier USS Nimitz (CVN-68) spent most of April isolated to prevent a viral outbreak before their scheduled deployment.
The Navy found enough COVID-19 test kits to help ensure no sailor with the Bremerton, Wash.-based Nimitz and the rest of Nimitz Carrier Strike Group would deploy infected with the virus that causes the COVID-19 disease. So teams with the Naval Health Research Center jumped in to help process the diagnostic tests for the deploying force of nearly 8,000.
At the time, the San Diego, Calif., based NHRC was in the midst of helping other ships and military treatment facilities process COVID-19 tests, a task that began Feb. 12. So far, “we have tested over 6,000 samples in total. That’s more than we did last year, all together,” Christopher Myers, the director of NHRC’s infectious diseases directorate, said during a media roundtable this week.
NHRC is testing 120 to 160 samples a day, officials said. While at that rate it couldn’t complete all processing of tests for big-deck ships such as Nimitz, Myers said, “we are operating seven days a week to support the requests that we get.” When the outbreak began, “we were one of the few options that the DoD had” to handle testing, he added.
The novel coronavirus – officially “severe acute respiratory syndrome coronavirus 2” or SARS-CoV-2 – causes the disease known as COVID-19. Infected people can suffer from mild-to-severe, flu-like symptoms including breathing difficulties, but the virus can be deadly. As of Thursday, almost 84,000 deaths in the U.S. were attributed to the virus, a jump of 1,701 from the day before, according to the Centers for Disease Control and Prevention.
The virus is detected through one of two ways: PCR or antibody.
A PCR, or polymerase chain reaction test or assay, identifies if any genetic material of the virus is present. It’s often collected through a nasal swab. An antibody test identities the presence of antibodies from an infection, and that’s done through blood tests. It can help track the virus spread and show someone’s prior infection, even if they don’t have symptoms.
Navy researchers have been using both tests, but for different reasons, supporting naval hospitals and the fleet as cases arose of coronavirus infections on several ships, including guided-missile destroyer USS Kidd (DDG-100) and littoral combat ship USS Coronado (LCS-4).
“NHRC mobilized to support the collection of nasopharyngeal swabs for PCR testing and blood samples for serology testing from both USS Kidd sailors and the Nimitz Strike Group,” spokesman John Marciano told USNI News. “NHRC rapidly created an outbreak response protocol and brought serology testing for antibodies to SARS-CoV-2 online.”
“There has been a lot of interest in serology testing,” Marciano said. “We’ve begun collecting blood samples from volunteers aboard the USS Kidd as part of an outbreak investigation aboard the ship. It’s not being used as a stand-alone diagnostic test, but when paired with PCR testing, it provides a better understanding of who may have been exposed to the virus.”

“We’ve been supporting the operational fleet as necessary and as directed to do so,” said Lt. Cmdr. Stephen Eggan, an infectious disease researcher. Once NHRC gets the samples to process, “we will run the tests and provide the results back to those health care professionals that took the samples,” Eggan said. The research center worked closely with Naval Medical Center San Diego to support testing for Kidd and Nimitz.
“What we’re using the serology testing for is to better understand the total prevalence within our military population, because PCR tells you whether or not you have the virus in you at this time in point. The serology tests can tell whether or not you’ve been exposed to the virus in the past,” said Eggan. “So we’re using the serology… to better understand the prevalence and spread within our Navy population.”
“We’re still very early on in what we are doing,” he added.
Patient testing hasn’t been a standard mission for NHRC, officials noted.
“We do not normally receive patient samples from the hospital. We are collecting them ourselves for surveillance,” Myers said. So “the whole process of the hospitals directly submitting samples to us and those results going into the medical records is a new process… We have the capability to do it, but we were doing it from a surveillance point of view,” not in helping make clinical diagnoses.
Since testing began in mid-February, NHRC has helped other military labs build testing capabilities, including the Pacific Rm Surveillance Hub in Yokosuka, Japan, Myers said. After the aircraft carrier USS Theodore Roosevelt (CVN-71) got detoured to Guam when scores of sailors became ill because of the coronavirus, NHRC jumped in to help. The western Pacific island is home to a sizable contingent of military personnel, but an influx of hundreds of infected sailors from a carrier would overwhelm existing medical capacities.

“We got a request from Naval Hospital Guam to help them stand up their own capability, and we’re able to provide manpower and supplies and training to get their own testing capabilities done and up and running,” Myers said. (Additional medical personnel along with other sailors and Marines with 3rd Medical Battalion, 3rd Marine Logistics Group, were deployed to Guam from Japan, bringing additional treatment to the naval hospital.)
NHRC teams also provided screening and testing for the hospital ship USNS Mercy (T-AH-19) before getting underway from San Diego to support local COVID-19 mission from the port of Los Angeles. “They wanted that ship to be clean when they started, so we helped them do some screen testing for the folks that were going onto the ship,” he said. “And most recently, we’ve done the reverse. As people are coming off the ship, we’ve cleared them for exit.”
NHRC is no stranger to pandemics. “We do have a lot of experience with this,” Myers said. “Starting in 2009, when we discovered the emerging (H1N1) pandemic in our surveillance efforts, we’ve been working with the CDC closely ever since.”
That year, NHRC researchers were the first to spot a new strain of the influenza virus in a young patient later identified as the H1N1 virus, aka the “swine flu.” The research center, using a CDC-approved PCR test, was the first DoD lab to confirm an H1N1 infection. For its work, NHRC received the CDC’s 2010 Excellence in Public Health Response Award.
“We were here on ground zero for the first one,” Myers said. “So we were working side by side with the CDC from day one of that from that virus being discovered… We were able to quickly respond to it and get things stood up and working.”
At the time, “there wasn’t a whole lot of flu testing going on,” he said. “That pandemic really drove the capabilities that we do have now. Back then, there were only two DoD labs that were able to support that. Now you are looking at 20, so we did learn a lot from that pandemic and a lot more capability has been pushed out.”
The infectious diseases directorate specializes in respiratory disease surveillance, making it well poised to support the COVID-19 outbreak, Myers said. But it’s not involved in developing a COVID-19 vaccine. “We don’t do that type of development and research here at my laboratory. We do have some partnerships with some others within the DOD that support that type of activity. Our samples and information will help support those studies,” he said.